According to the Fresno County Department of Public health, the total number of cases in Coalinga, as of 4 PM today, was 76. Total cases include all cases incurred and each person is only counted once even if they have more than one positive test.
Our first positive case was on April 9, 2020. Our most recent positive case was today.
Cases are closed one of three ways:
- Non-Lab Method (symptom free for 3 days)
- Automatic close after 10 days from the disease onset date
- Lab Cleared (a negative test result).
Those identified as being ‘positive with close contact‘ mean the Fresno County Department of Public Health has identified the source of where the person contracted the disease.
Community spread/unknown refers to cases when the Fresno County Department of Public Health cannot identify the specific source of where the person contracted the disease. This could be from having contact with someone in the community who was positive.
Travel related are those who have traveled to a different county. For example, someone went to the beach or took a trip out of the county and shortly thereafter began feeling sick.
Those cases that are listed as under investigation mean that a contact tracer has been assigned. Contact tracers are specially trained individuals who have learned to backtrack a person’s interaction with others, and where those interactions occurred.
Our data as of 4:00 PM today was as follows:
- 76 total cases (25 resolved and 51 active)
- 19 were contracted through close contact
- 16 were community spread
- 4 were travel related
- 37 are under investigation
Within our 76 cases, none have been inmates at Pleasant Valley State Prison. Two have been patients at the Coalinga State Hospital but those cases are both no longer active.
The biggest jump in positive cases was from June 3, 2020, to June 30, 2020 as we had a 60 case increase.
This liaison stated that we have had zero COVID-19 deaths. He further stated that if a person with COVID-19 passes away from something such as Pneumonia or a heart attack, the death certificate will list the Pneumonia or heart attack as the cause of death, not COVID-19 if COVID-19 was not the actual cause.
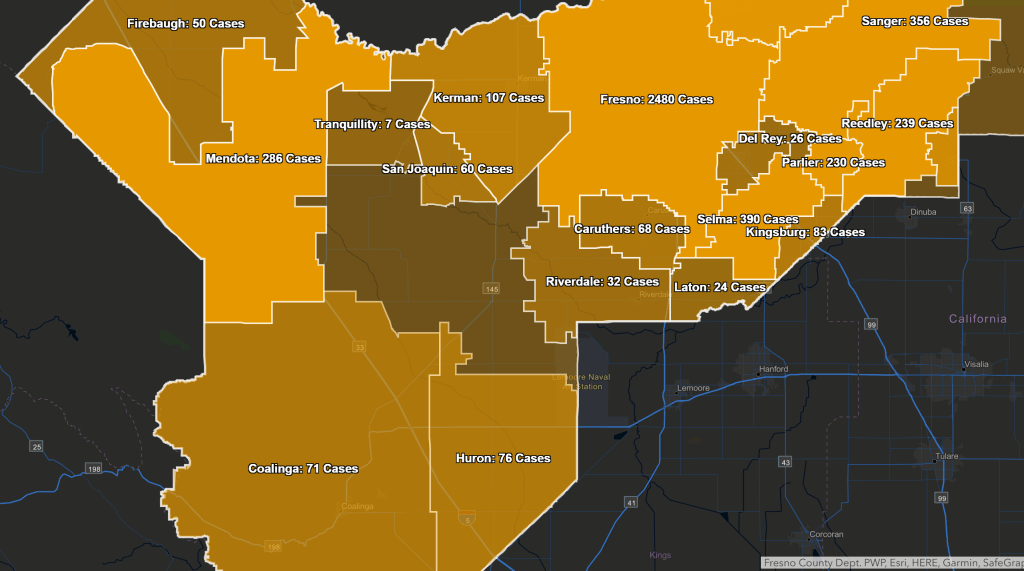
The liaison will be providing Coalinga’s City Manager, marissa Trejo, with a ‘heat map’ indicating the areas of the City with positive cases.
There is a general information number that anyone can call Monday-Friday from 8:00am to 5:00pm. That number is 559-600-3332. After hours, a person could call 211.
The FCDPH stated there are no testing sites in Coalinga and provided the following link to find a testing site: https://www.co.fresno.ca.us/…/covid-…/covid-19-testing-sites
Residents can also sign up for testing on this website.

Governor Newsom Mandates Reversing Some Openings
Guidance on Closure of Sectors in Response to COVID-19
July 1, 2020
Summary
As COVID-19 transmission rates continue to rise, this guidance instructs counties that have been on the County Monitoring List for three consecutive days or more to close indoor operations for certain sectors which promote the mixing of populations beyond households and make adherence to physical distancing with face coverings difficult. Within those sectors, those that are not able to continue their business through outdoor operations must close that portion of their business effective immediately for at least three (3) weeks, in order to further mitigate the spread of the virus. In addition, all brewpubs, breweries, bars, and pubs in these counties must close, both indoors and outdoors.
Background
As part of the State’s efforts to address COVID-19, the State monitors county specific data and provides technical assistance, support and interventions to counties that have concerning levels of disease transmission, hospitalizations, or insufficient testing. Counties on the County Monitoring List are under active monitoring by the state, and may receive targeted engagement and technical support from CDPH and other agencies and departments including the Business, Consumer Services and Housing Agency, the Department of Industrial Relations and the California Department of Food and Agriculture.
As of July 1, there are 19 counties on the County Monitoring List, which includes:
• Contra Costa
• Fresno
• Glenn
• Imperial
• Kern
• Kings
• Los Angeles
• Merced
• Orange
• Riverside
• Sacramento
• San Bernardino
• San Joaquin
• Santa Barbara
• Santa Clara
• Solano
• Stanislaus
• Tulare
• Ventura
To reduce disease transmission and to protect residents across the state, one strategy available to the state is to work with counties to further modify or close some or all of the sector openings currently allowed under the State order.
Proposed Action
Given current rates of disease transmission in some counties and the need to reduce gatherings where mixing with individuals outside of one’s household and disease spread occur, CDPH is requiring closure, within counties on the county monitoring list for three or more consecutive days, of indoor operations, while allowing outdoor operations with appropriate modifications, including physical distancing and face coverings, for the following sectors:
• Dine-in Restaurants
• Wineries and Tasting Rooms
• Movie Theaters
• Family Entertainment Centers
• Zoos and Museums
• Cardrooms
All industry or sector guidance documents that have been issued to date, including all infectious control measures outlined in those guidance documents, apply in outdoor settings, and thus must be adhered to. In addition, all brewpubs, breweries, bars, and pubs must close indoor and outdoor operations in these counties.
Justification
The data is clear that community spread of infection is of increasing concern across the state, and in particular for those counties on the County Monitoring List. Beyond the impact on the general population, community spread increases the likelihood of expanded transmission of COVID-19 in congregate settings such as nursing homes, homeless shelters, jails and prisons. Infection of vulnerable populations in these settings can be catastrophic, both in terms of high rates of morbidity and mortality of individual residents, as well as through the high demand such infections would place on the hospital delivery system. We are seeing these increases already in many of the counties. Higher levels of community spread also increase the likelihood of infection among individuals at high risk of serious outcomes from COVID-19, including the elderly and those with underlying health conditions who might live or otherwise interact with an infected individual.
California’s Pandemic Resiliency Roadmap for reopening is a risk-based framework that guides state and local governments on a path to re-opening industries under strict workplace modifications. Whereas other industries and establishments were permitted to open with modifications in Stage 2 or Stage 3, the above outlined sectors operating indoors operate at the highest risk of all sectors allowed to open so far. These specific sectors also create an environment that increases levels of community mixing of individuals outside of one’s own household, increasing the risk of escalating the R-effective, or effective transmission rate, of COVID-19.
The sectors at issue in this document are all high risk of transmission due to a number of features of the businesses and the behaviors that occur within them. These sectors, foundationally, are settings where groups convene and may mix with others for prolonged periods of time without appropriate protective equipment, such as a face covering. For example, it is difficult to consistently wear a face covering in a restaurant. Additionally, physical movement within the establishment, duration of time spent in the establishment, and the degree of social mixing among individuals and groups outside one’s household are all significant in these sectors, which substantially elevates the risk of transmission even where face coverings can be worn.
The risk is particularly high in indoor settings. Reinstituting indoor closures among these sectors is not only important because of data from counties on the monitoring list, but because the science of disease transmission and from recent studies have shown that the transmissions is greater in indoor settings due to the release of infectious particles into the air when someone speaks, coughs, sneezes, or sings, which is exacerbated in indoor spaces particularly when lacking appropriate ventilation. Furthermore, in some of these sectors centered on eating and drinking, compliance with face coverings is not possible for the full duration of time someone spends in these establishments. Additionally, the workforce of these sectors face higher exposure to diseases transmission because of the environment in which they work.
A recent study published by the Centers for Disease Control and Prevention, for example, demonstrates clearly the effect of a single asymptomatic carrier in a restaurant environment. The study shows that approximately 50 percent of the people at the infected person’s table become sick over seven (7) days, 75 percent of the people on the adjacent table that is downwind in the interior ventilation system become infected, and even two of seven people on the upwind table become infected. (1)
Physical distancing also protects an individual with brief exposures or outdoor exposures. When distanced, there is not enough time to achieve the infectious viral load when standing six (6) feet apart or where wind and the infinite outdoor space for viral dilution reduces viral load. A study, which still needs to be peer-reviewed, suggests that the odds an infected person transmitting the virus in a closed environment was 18.7 times greater compared to an open-air environment. (2)
Alcohol consumption slows brain activity, reduces inhibition, and impairs judgment, factors which contribute to reduced compliance with recommended core personal protective measures, such as the mandatory use of face coverings and maintaining six feet of distance from people outside of one’s own household, making outdoor operations for brewpubs, breweries, bars, and pubs challenging, further creating opportunities for virus transmission and thus need for closure. Additionally, there is a growing body of evidence tracing large COVID-19 outbreaks in both urban and rural states, to indoor and outdoor operations of bars.
In the setting of an increasing body of evidence demonstrating that transmission is decreased when activities are conducted outside, and risk for exposure is increased when mixing beyond those with whom one lives, in an effort to mitigate to potential spread of COVID 19, the state is requiring that settings where patrons gather to be served or participate in the businesses’ primary activity be moved outdoors.
(1) Lu, J., Gu, J., Li, K., Xu, C., Su, W., Lai, Z….Yang, Z. (2020). COVID-19 Outbreak Associated with Air Conditioning in Restaurant, Guangzhou, China, 2020. Emerging Infectious Diseases, 26(7), 1628-1631. https://dx.doi.org/10.3201/eid2607.200764.
(2) Nishiura et al. (2020). Closed environments facilitate secondary transmission of coronavirus disease 2019 (COVID-19). https://www.medrxiv.org/content/10.1101/2020.02.28.20029272v2.

California Department of Public Health
PO Box, 997377, MS 0500, Sacramento, CA 95899-7377
Department Website (cdph.ca.gov)